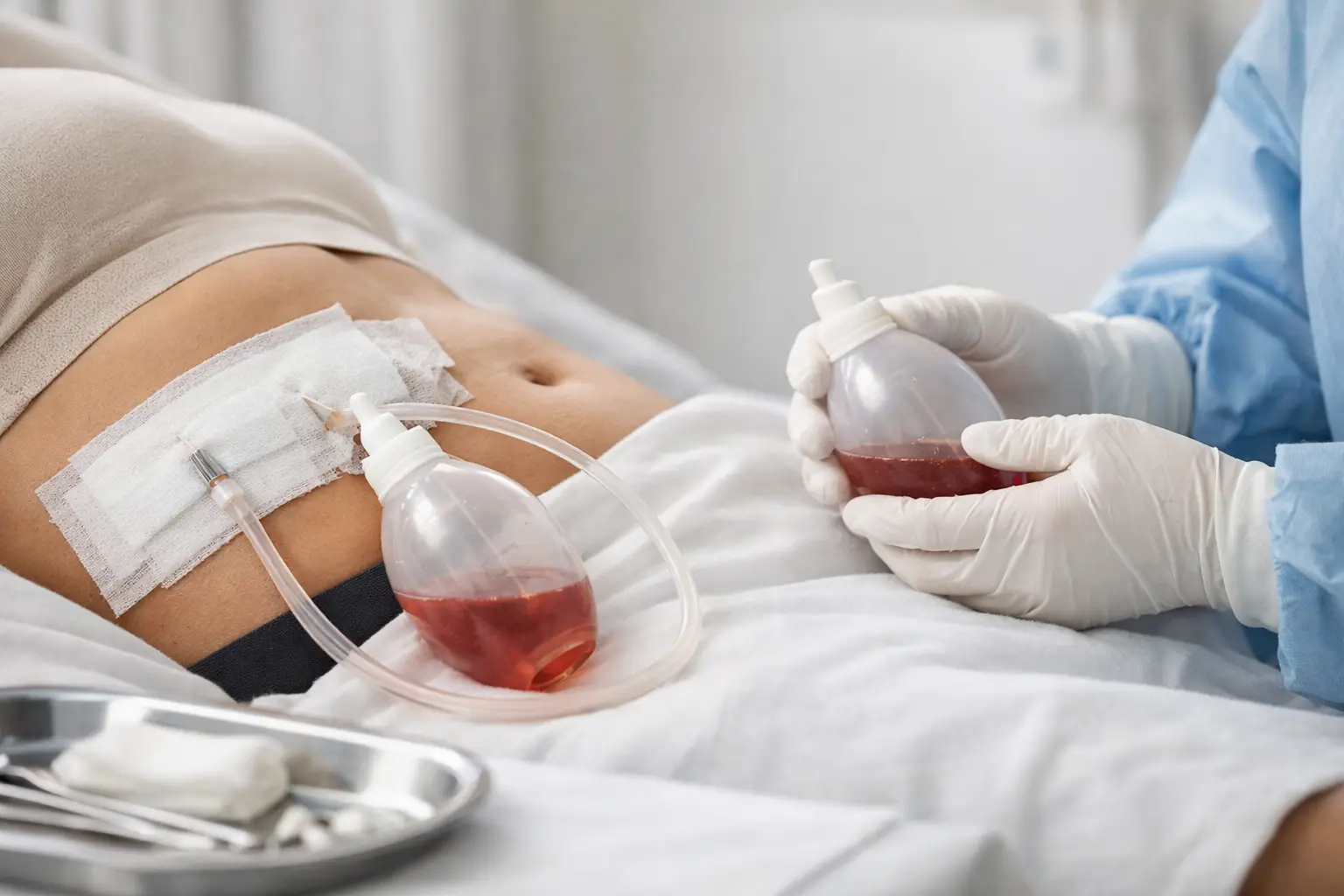
The days following surgery often mix relief, anxiety, and numerous questions. It is precisely in this phase that understanding how to care for the post-operative period makes a difference in swelling, comfort, healing, and even the final aesthetic result.
Each surgery has its peculiarities, and the surgeon's guidance always comes first. Nonetheless, there are basic care steps that help most patients navigate this phase with more security, less discomfort, and a more organized recovery.
Practical Post-Surgery Care
Post-surgery care isn't just about waiting for your body to 'heal itself.' The body is dealing with inflammation, fluid retention, sensitivity, movement limitations, and often, a routine completely different from usual. Consistent daily care is essential.
Rest is crucial, but resting doesn't mean abandoning your recovery routine. In many cases, staying immobile for too long may not be ideal. Light movements, position changes, and small walks, when approved by your doctor, often aid circulation and reduce body heaviness.
Hydration also plays a key role. Drinking water throughout the day supports bodily functions and can help manage swelling. When nutrition is added to this equation, the scenario improves even more. Balanced meals, rich in proteins, vegetables, greens, and minimized sodium, tend to aid the healing process and reduce swelling.
Another crucial point is following medical prescriptions accurately. This includes medication schedules, use of compression garments, proper bandage care, and attending follow-up visits as scheduled. It seems basic, but much post-operative discomfort begins when patients feel better and slack off on care that still needs to continue.
Factors Influencing Recovery
A smooth recovery usually depends on a set of factors. While the type of surgery matters, it's not the only element. Each person's body reacts differently to surgical trauma, which explains why two patients with the same procedure might experience different levels of swelling, pain, and recovery time.
Sleep, for instance, is often underestimated. Poor sleep increases body stress and may affect the perception of pain and fatigue. Sleep position also deserves special attention, as some surgeries require specific postures to avoid pressure on the operated area. Improvising is not a good idea in these cases.
Additionally, it is worth noting the home environment and routine. Having support in the initial days, keeping frequently used items within reach, and avoiding heavy lifting or housework is more than comfort—it's genuine care for recovery.
Swelling, Pain, and Sensitivity: What to Expect
A common question is knowing how to distinguish normal symptoms. Swelling, tightness, bruising, and sensitivity are part of the process, especially in the first weeks. This doesn't mean everything should be ignored, but rather that the body is reacting to the procedure.
The focus should be on intensity, progression, and associated signs. Worsening pain, fever, intense redness, excessive warmth in the area, foul-smelling discharge, or shortness of breath require immediate medical contact. Meanwhile, moderate swelling that gradually improves is generally within expectations.
Lymphatic Drainage Post-Surgery: When It Makes Sense
In many surgeries, post-operative lymphatic drainage can be an important ally in reducing swelling, enhancing local circulation, and facilitating a more comfortable recovery. However, an essential aspect here is that it's not just any massage or any timing.
Care must be tailored to the tissue stage, medical clearance, and appropriate post-operative techniques. Intense movements, incorrect pressure, or uninformed approaches can increase sensitivity and disrupt the process, rather than aiding it.
When properly indicated, drainage contributes to a well-monitored post-op period. Many patients report feeling lighter, with reduced swelling and improved mobility over sessions. The ideal number and frequency depend on the specific procedure, body response, and professional assessment.
For those seeking such support in Brasília, especially in Vicente Pires, having specialized post-op drainage care makes a difference, as the care becomes personalized and considers the body's actual state.
How to Care for Post-Surgery Without Hindering Healing
Some mistakes are more common than they seem. The first is rushing to achieve the final result. Anxiety leads many patients to try self-made solutions, apply compresses without guidance, stop wearing compression garments too soon, or resume physical activities prematurely. In recovery, haste often comes at a high cost.
Another frequent mistake is comparing personal progress with others. Before-and-after photos, social media experiences, and friends' stories can create distorted expectations. The body has its own pace, and healing doesn't always follow a visually linear timeline.
It's also important to avoid unnecessary handling of the operated area. Pressing to 'check for swelling,' constantly touching the scar, or carelessly sleeping because you feel better can irritate the area and prolong discomfort. The post-op period demands discipline even in the details.
The Role of Compression Garments, Posture, and Routine
Compression garments, when indicated, assist in containment, tissue support, and swelling control. But for them to work effectively, they need to be correctly fitted to your body and worn for the recommended duration. A garment that is too tight can be uncomfortable and leave marks; one that's too loose loses its function.
Posture also plays a significant role. Getting up, sitting, and lying down abruptly can strain the operated area. In some cases, keeping the chest slightly elevated or avoiding certain positions while sleeping helps reduce pressure and pain. These are simple adjustments but can have a cumulative positive effect over time.
In daily life, simplifying as much as possible is wise. Postponing unnecessary commitments, accepting help, and respecting one's own limits is often more intelligent than trying to prove resilience. A good recovery isn't the quickest in appearance— it's one that occurs safely and stably.
When to Seek Professional Help Beyond the Surgeon
The surgeon is the primary reference during the post-op phase, but this doesn't rule out supplementary support from skilled professionals. In many cases, such assistance makes recovery more comfortable and monitored, especially when there is persistent swelling, a feeling of tissue hardening, or the need for more targeted care.
In the aesthetic and therapeutic areas, the key is to adapt techniques to the patient's current stage. An operated body cannot be treated like a body undergoing regular treatment. Evaluation, listening, and technical precision matter significantly.
Supportive care also counts a lot. Post-operative patients are usually more sensitive, more tired, and sometimes insecure about their bodies. Being accompanied by a professional who understands this scenario and works methodically is a significant part of the recovery experience.
What to Expect in the First Few Weeks
The first weeks are often full of fluctuations. One day, your body might respond well; the next, swelling might increase a bit or sensitivity might change. This happens and doesn’t always indicate a problem. Recovery rarely follows a straight line.
The most important thing is observing trends, not just an isolated day. If there's gradual improvement, even with small variations, the process tends to progress adequately. If there's continual worsening or symptoms outside the normal range specified by your doctor, it's time to reassess.
Be patient with the mirror. The final result isn't visible at the beginning, and the swelling phase can significantly skew the perception of surgery. Good post-operative care often means accepting that the body needs time to deflate, reorganize tissues, and show the results more authentically.
The best care combines medical guidance, consistent routine, and technical monitoring when indicated. When these elements align, recovery tends to be smoother, safer, and far more respectful to your body.